A successful IVF treatment is a pregnancy that results in the birth of a healthy child. Many aspects are discussed in order to raise pregnancy rates. An increasingly important parameter to reflect a successful IVF program in today's world of IVF is the time to pregnancy and live birth. In this blog post I will go through some of the critical steps in the IVF procedure and how they can be optimised.
Three parts influence a successful outcome
The chance of success is influenced by three major parts;
- Patient
- Physician
- Laboratory
The patient and the physician are determining factors in the beginning (stimulation and oocyte retrieval) and at the end (transfer and endometrium receptivity) during the clinical part of the IVF treatment.
The laboratory is in between and has a major impact on the entire IVF procedure chain. Here, gametes are handled and by using an individualised approach the laboratory staff will find the best ways to obtain and grow embryos in-vitro, as well as identify embryos with the highest implantation potential.
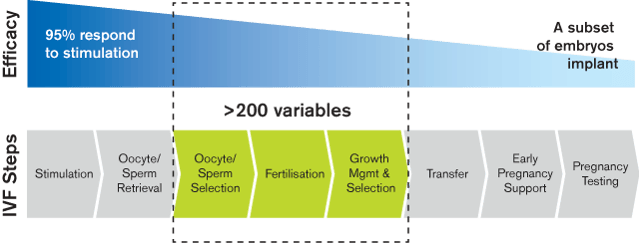
In the laboratory, the number of variables that can influence the success is huge. The challenge is to be aware of all these variables and to know how to control them in order to be able to offer the best treatment possible under the given conditions.
The IVF laboratory is the place, where most variables that may affect the outcome of an IVF treatment are present. The image above illustrates the need for strict quality control and quality management in order to maintain a high consistency in the daily work.
Absolute essentials that impact outcome
Among the variables that mostly impact the laboratory outcome, the control of the ones listed below must be considered as absolute essential.
Oocyte retrieval
- Preparation of dishes
- Temperature / Osmolality
Culture
- pH / CO2 / Temperature / Handling
- O2 / Day 5
Reprotoxicity
- Labware, media
- Air quality
Infrastructure
- Laboratory set-up
- Procedure chain
Human resources
- Staff
- Education & knowledge
Oocyte retrieval
The oocyte retrieval procedures involves much more than the actual pick-up. The work in the lab starts with preparation of dishes on the day before pick-up. A non-appropriate dish preparation method can set the stage for an osmolality shock, due to evaporation.
The same applies to the pick-up process, where missing temperature control can damage the cytoskeleton of the oocyte. An impact at such an early stage will reduce the stress tolerance for later embryo development. Learn more about temperature control in this blog post.
Culture
There are many factors affecting culture of oocytes and embryos. Most of these can be controlled by proper awareness. Avoiding unnecessary incubator door openings is a must to maintain stable and undisturbed culture conditions, and the optimal culture system is an integrated time-lapse incubator.
pH, temperature and culture at reduced oxygen are the key parameters for embryo development, independent of if you aim for day 2, day 3 or day 5 transfer.

Embryos can tolerate a lot of stress and still show a decent development. However, stress can accumulate and impacts the potential to implant as well as the course of the pregnancy.
Reprotoxicity
Toxicity can be introduced in the process of an IVF treatment and needs to be taken care of. Not all products we use in IVF are optimised for this application. Therefore it is important to insist on proper quality control from the manufacturer and provider of IVF products and also ask about how products are tested and released.
Once in house, the proper environment in terms of air quality must be provided during culture. Volatile organic compounds (VOCs) are an easily overlooked and undetected cause for suboptimal conditions. VOCs can be measured and air quality can be maintained with proper filtration systems or incubation systems. Read more about how to secure air quality in the lab here.
Infrastructure
A proper infrastructure is more than just having an IVF laboratory with the required equipment. The laboratory must have a suitable and ergonomic set-up with restricted entry and proper storage of products according to their needs. Standard operation procedures (SOPs) must be in place for the entire procedure chain. The needs and requirements of the laboratory also need to be overlooked.
A laboratory is not carved in stone once it is up and running. New procedures will be adapted, space will become limiting at some point and equipment must be upgraded. A proper strategy right from the beginning is mandatory.
Human resources
Human resources are often a neglected entity, however, it should be one of the easiest to control. IVF is a teamwork, which involves everyone working in a clinical ART centre. A happy and well-staffed team is a successful team because the communication level is high, which prevents misunderstandings. Constant exchange and continuous education is a motivation factor that should not be underestimated.

Embryologists need interaction to bring everyone to the same level and align on decisions and assessment strategies. Objective supporting tools, eg for embryo evaluation, can support discussions, knowledge sharing and the evolution of standardisation.
Learn more
At ESHRE I held a presentation at the Vitrolife Scientific Symposium with the same topic as this blog post, where I went through the above steps more in detail. Click below to watch this presentation.
Topics: IVF laboratory control, Embryo culture & transfer
Written by Dr. Markus Montag
Markus is a well-known researcher in the field of IVF, where one of his specialities is time-lapse. He has more than 20 years’ experience as Lab Director. Markus spends his time working as a consultant for IVF centres around the world and also for Vitrolife.
